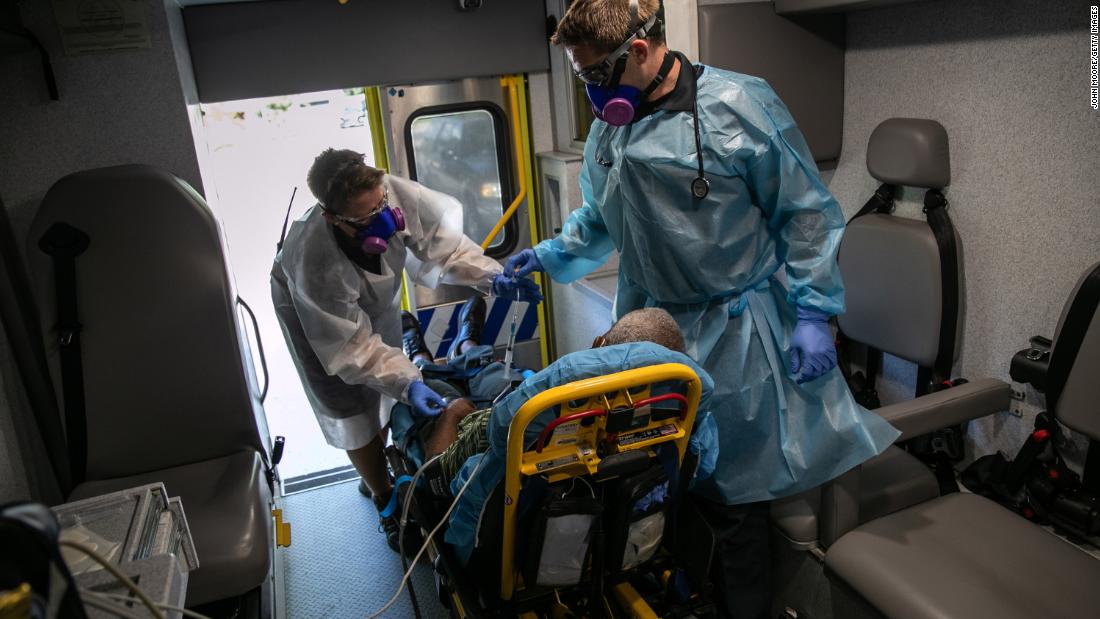
Covid-19 data confirms what experts have suspected about what influences whether you live, die or get help
“What Covid-19 does is actually shine a light on a problem that was already there,” said Dr. Lisa Cooper, director of the Johns Hopkins Center for Health Equity.
Race affects who is able to flee from a viral hotspot to a second home and who shares a roof with family members across generations. It affects who is able to work remotely and who has to leave home to keep society afloat. It affects who has easy access to testing and who puts off treatment because they’re worried about the costs.
In other words, as the US approaches six million confirmed coronavirus cases, race plays a major role in who lives, who dies and who gets help.
Race affects where you live
The advice from health experts has been constant: Maintain physical distance from others to avoid contracting the virus.
But for many marginalized groups, that’s easier said than done.

Medics transport a man with possible Covid-19 symptoms to the hospital on August 7 in Austin, Texas. African Americans continue to be disproportionally affected by the coronavirus pandemic.
“We’re talking about housing that is probably older and poorer quality,” Cooper told CNN. “It’s smaller rooms in homes that don’t have several bathrooms.”
She cited a Covid-19 patient she spoke to who worked in hotel housekeeping. The patient’s family shared a house with one bathroom, and everyone in her family ended up getting infected. The woman’s husband died of the virus, Cooper said.
“In normal times, it’s a coping strategy, a way to be able to survive and do quite well with limited incomes,” Capps said. “But in this environment, it can be problematic.”
The region is now a coronavirus hotspot, and essential farm workers, Latinos and those living in shared housing — groups that often overlap with each other — are being disproportionately infected, Gov. Gavin Newsom said last month.
Multigenerational homes are a frequent reality for American Indians and Alaska Natives too, said Stacy Bohlen, chief executive officer of the National Indian Health Board and a member of the Sault Ste. Marie Tribe of Chippewa Indians.
“You take into account very poor housing for our folks,” she said. “And yet we hold family as a top priority for the way that we approach the world.”
That means there might be several generations living in a house designed for four people, Bohlen said. Add to that the lack of running water, sewage and sanitation facilities on some tribal lands, and even complying with basic hand-washing guidance can be challenging.
“If you look at the history and you look at where we find ourselves, there’s no way else it could have played out,” she said.
It affects whether you can work from home
Another commonly cited piece of coronavirus safety advice: Stay home.
Black and Hispanic workers in the United States are “much less likely” to be able to work from home, economists Heidi Shierholz and Elise Gould wrote in a post in March.
Those discrepancies have to do with “occupational segregation by race and ethnicity,” Shierholz told CNN at the time.


Farm laborers harvest romaine lettuce on a machine with heavy plastic dividers that separate workers from each other on April 27, in Greenfield, California.
That means they’re more likely to be exposed to the virus while on the job — if they still have one.
Black and Latino people are also more likely to rely on public transportation, and may need to make more frequent trips to the store because they can’t afford to stock up, Cooper said.
It affects your risk of severe illness
Even before they get infected, many people of color face heightened risks.


A patient is taken from an ambulance to the emergency room of a hospital in the Navajo Nation town of Tuba City, Arizona, on May 24, 2020.
“It’s like double jeopardy right now,” Cooper said.
It affects your access to medical care
When people of color get infected, they don’t always get the treatment they need.
Black and Latino Americans are more likely than White people to lack health insurance and tend to put off seeking care, according to the National Urban League report. So by the time they see a health care provider, they are sicker.
“With that, it’s not surprising that people are going to not believe what they’re hearing from experts, or be afraid that they’re going to be harmed in some way,” Cooper said.
“That is so grossly underfunded that the joke in Indian Country used to be, ‘Don’t get sick after June 1,'” Bohlen said. “Because appropriations begin October 1 and by June 1, all that money for specialty care is gone.”
Another barrier that Native Americans face, lack of broadband access, affects their ability to receive updated public health information and participate in telemedicine calls.
How we move forward
The systemic barriers that contribute to the racial disparities around Covid-19 are deeply rooted and cannot be easily reversed. They stem from longstanding inequities in housing, education, employment and other sectors.
“There’s just layers and layers of issues that have led to extreme social disadvantage in those communities,” Cooper said.
Still, organizations that advocate for Black, Latino and Native Americans have been working during the pandemic to make sure their communities get the support they need.


Medical workers hold signs during a rally, organized by a group named White Coats for Black Lives, on June 6 in New York.
These problems are big and demand big solutions, advocates say. Unraveling them will require peeling back the layers and committing to addressing it, piece by piece.
CNN’s Catherine Shoichet contributed to this report.
![]()